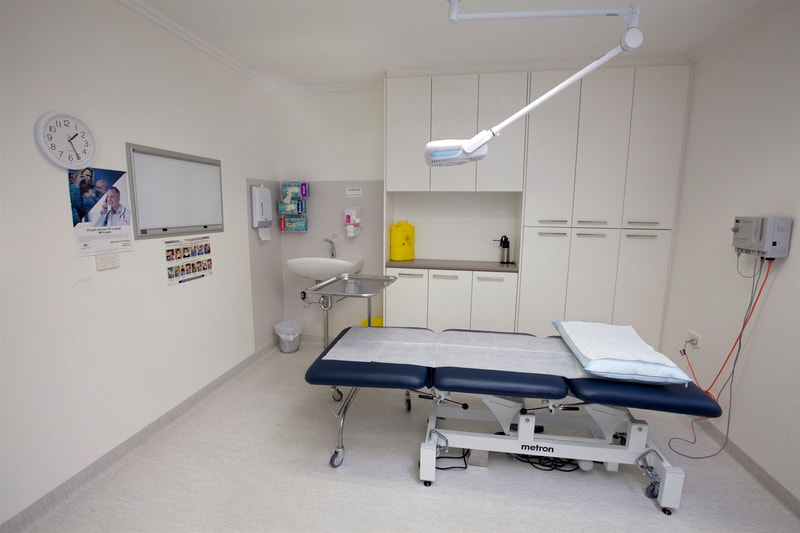
What is Specialist General Practice
General practice in Australia has been a speciality since 1996. As a specialist practice, a doctor could not just set up a general practice after one or two years as a junior doctor. All doctors wanting to work in general practice had to undertake specialist training and complete a fellowship (specialist qualification in medicine). One must pass a difficult set of standardised, validated assessment examinations and awarded a fellowship in general practice (Fellowship of the Royal Australian College of General Practitioners or FRACGP). This qualification is a specialist medical qualification and is recognised by the Medical Council of Australia as such.
Definition of specialist general practice
Specialist general practice is whole-person care, characterised by the provision of person-centred, continuing and comprehensive medical care to individuals and families in their communities. As a relationship-based discipline, the general practice seeks to build health, wellbeing and resilience through a continuing patient‐doctor relationship of trust, clinical acumen, the application of best available evidence in the unique context of each consultation, and planned coordination of clinical teamwork, resources and services. The patient’s needs, values and desired health outcomes always remain central to the general practitioner’s evaluation and management processes.
|
Person centredness
General practitioners understand that health, illness and disease are ultimately personal experiences. Their principal role is to relieve illness in all its forms, in the manner best suited to each individual. |
Continuity of care
Long‐term relationships build mutual knowledge, understanding, experience and trust: all essential elements in a therapeutic relationship, which generates the potential for healing, increased resilience, empowerment and beneficial change. |
|
Comprehensiveness
General practice is not limited by age, gender, body system, disease process or service site. The scope of practice is forever challenging its practitioners. It spans prevention, health promotion, early intervention for those at risk, and the management of acute, chronic and complex conditions, whether in the home, practice, health service, outreach clinic, hospital or community. |
Diagnostic and therapeutic skill
The general practitioner's high level diagnostic and therapeutic skills as applied in the context of person-centred and continuing relationship is known to deliver safe, high-quality, and cost-effective care that is highly valued by patients. |
|
A command of complexity and uncertainty
General practitioners are comfortable with uncertainty and skilled in managing complexity. They can utilise best practice evidence in the light of individual patient circumstances. They engage patients, parents and families in understanding, planning and better managing their health according to their capacities. |
Coordinated clinical teamwork
General practitioners work in close and respectful relationships to deliver integrated patient care. Leading, supporting and coordinating their flexibly configured clinical teams; contributing appropriately to external clinical teams, and collaborating with a diversity of community-based professionals – according to the individual patient or family's needs and circumstances. |
-
People
-
Mission Statement
-
Your Privacy
-
Patient Access to Medical Records
<
>
Contracting Doctors @ gpmaroubra
|
Dr Shane Christensen
MBCHB; FRACGP; MPH&TM; GCMEDED Contracting Practice Principal & Clinical Director Specialist General Practitioner Clinical Associate UNSW & University of Sydney Medical Educator GP Supervisors (GP Synergy) |
Dr Amanda Garcia
BMEDSC; MBBS; FRACGP; DCH Contracting Practice Associate Specialist General Practitioner |
Dr Simon Howell
FRACGP; BSc MChiro BHealthSc MBBS Hons; GradCert Med Ed; Clin Dip Palliative Medicine Contracting Practice Associate Specialist General Practitioner |
|
Dr Merissa Cappetta
BMEDSC; MBBS; FRACGP; FAChAM Contracting Practice Associate Specialist General Practitioner Dr Lynsey McHugh
MBChB Practice Associate Registrar General Practitioner |
Dr Amanda Henderson
MBBS; FRACGP Contracting Practice Associate Specialist General Practitioner |
Dr William Stewart
MBBS; FRACGP Contracting Practice Associate Specialist General Practitioner |
Nurses
Practice Manager
Reception Staff
Mission Statement
gpmaroubra is a specialist primary care clinic committed to providing outstanding health care to individuals and the community. We are dedicated to providing excellence in professional medical training for students and junior doctors.
Here at gpmaroubra, we meet the health needs of people at the highest standards and ensure that each patient spends enough time with a contracting doctor or nurse in the delivery of health care.
We are not a medical centre. We are a medical home for people where all your healthcare needs are coordinated. Contracting doctors deliver outstanding healthcare by providing: excellence in medical knowledge and excellence in communication. All contracting doctors have or are in the final year of gaining their specialist fellowship in general practice: the FRACGP.
Our team at gpmaroubra is passionate about the delivery of high-quality whole-person primary care through a collaborative model of medical practice. This means we all work together: reception, managers, nurses and contracting doctors, to give people the best possible health outcomes.
Specialist general practice involves an in-depth knowledge of medicine and an integrated understanding of all aspects of a person’s life that determines their health and wellbeing. This whole-person care addresses the psychological, social, spiritual, nutritional, environmental and physical dimensions of a person’s health and wellbeing.
At gpmaroubra staff and contracting doctors are committed to the highest standards of professional development, including the enthusiastic teaching and training of medical students and junior doctors.
gpmaroubra provides a supportive and stimulating work environment that promotes an interactive and collaborative relationship amongst us all, including staff and contracting doctors.
To deliver the highest quality health care and clinical training, we are committed to a set of core values.
Here at gpmaroubra, we meet the health needs of people at the highest standards and ensure that each patient spends enough time with a contracting doctor or nurse in the delivery of health care.
We are not a medical centre. We are a medical home for people where all your healthcare needs are coordinated. Contracting doctors deliver outstanding healthcare by providing: excellence in medical knowledge and excellence in communication. All contracting doctors have or are in the final year of gaining their specialist fellowship in general practice: the FRACGP.
Our team at gpmaroubra is passionate about the delivery of high-quality whole-person primary care through a collaborative model of medical practice. This means we all work together: reception, managers, nurses and contracting doctors, to give people the best possible health outcomes.
Specialist general practice involves an in-depth knowledge of medicine and an integrated understanding of all aspects of a person’s life that determines their health and wellbeing. This whole-person care addresses the psychological, social, spiritual, nutritional, environmental and physical dimensions of a person’s health and wellbeing.
At gpmaroubra staff and contracting doctors are committed to the highest standards of professional development, including the enthusiastic teaching and training of medical students and junior doctors.
gpmaroubra provides a supportive and stimulating work environment that promotes an interactive and collaborative relationship amongst us all, including staff and contracting doctors.
To deliver the highest quality health care and clinical training, we are committed to a set of core values.
- Best Practice
We work collaboratively with each other and our medical and allied health colleagues. This best practice ensures staff and contracting doctors do deliver evidence-based and patient-centered health care, specific to the needs of individual patients. gpmaroubra reflects this core value in the teaching and learning undertaken with all our students and junior doctors. - Priority
The care of patients is the highest priority to our staff and contracting doctors. - Commitment
to excellence in health care and clinical teaching by staff and contracting doctors. - Confidentiality
is respected for all patients, contracting doctors and staff. - Care and Compassion
is shown to all patients, contracting doctors, staff and students - Collaboration
We collaborate with patients, each other, other health care providers and teaching centers to provide the best possible environment for our patients, staff, contracting doctors and students. - Communication
We have outstanding communication with patients, each other, other health care providers and teaching centres. - Competence
We ensure the highest level of competency in all our work. - Integrity
Integrity in everything we do at gpmaroubra ensures we are ethical, honest and transparent. - Responsibility
Responsibility is taken for our actions as individuals and as an organisation. - Advocacy
We advocate the best possible health care delivery to our patients by our staff and contracting doctors.
Your Privacy
This practice is committed to providing quality health care and service. As part of this, we have the policy to protect your privacy that complies with privacy legislation*
This policy protects all health information that is collected and used by this practice.
Our Privacy Policy advises you:
We ask that you assist us in providing the best possible health care to you by making sure that the information we have is accurate and up to date.
Ask your doctor or see our reception staff if you would like more information about our Privacy Policy or the National Privacy Principles and Health Records and Information Privacy Act, 2002.
*Privacy Amendment (Private Sector) Act 2000; HRIP Act 2002.
This policy protects all health information that is collected and used by this practice.
Our Privacy Policy advises you:
- That we need your consent to collect information about you
- That you can request access to the information, we hold about you.
- That you may discuss any concerns that you have about how we handle your data with your doctor or the practice staff.
- How your information will be used by us and whom we may need to disclose it. This may include an organisation assisting in improving the administration of the practice.
We ask that you assist us in providing the best possible health care to you by making sure that the information we have is accurate and up to date.
Ask your doctor or see our reception staff if you would like more information about our Privacy Policy or the National Privacy Principles and Health Records and Information Privacy Act, 2002.
*Privacy Amendment (Private Sector) Act 2000; HRIP Act 2002.
Patient Access to Medical Records
It is practice policy that all patients have access to the health information contained in their file. Access may be denied if access is deemed to present a serious health threat to the individual’s health or when the privacy of another individual may be compromised. If this is the case their treating doctor will provide them with an up to date and accurate summary of their health information on request.
Should a patient want to access their health records they should speak to the Practice Manager or their treating doctor.
Personal health information may be accessed in the following ways:
Note: For information that is posted, a cost may be incurred by the patient.
Should a patient want to access their health records they should speak to the Practice Manager or their treating doctor.
Personal health information may be accessed in the following ways:
- View and inspect information
- View, inspect and talk through contents with the doctor
- Take notes
- Obtain a copy (can be photocopy or electronic printout from computer)
- Information may be faxed to patient (with patient being aware that this is not a secure method of private information transmission) or posted.
Note: For information that is posted, a cost may be incurred by the patient.